In clinics and charts around the world, a simple height-and-weight formula continues to guide decisions about health, often without telling the whole story.
Body Mass Index, or BMI, is one of the most widely used tools for assessing body size in healthcare and public health. Developed as a simple calculation based on height and weight, it has long been used to categorize individuals into weight ranges associated with potential health risks.
However, while BMI can offer useful population-level insights, it has important limitations when applied to individuals. Understanding what BMI is—and what it isn’t—can help you interpret it more accurately and make more informed decisions about your health.
What Is BMI?
BMI, or Body Mass Index, is a numerical value calculated using a person’s weight and height. The formula is:
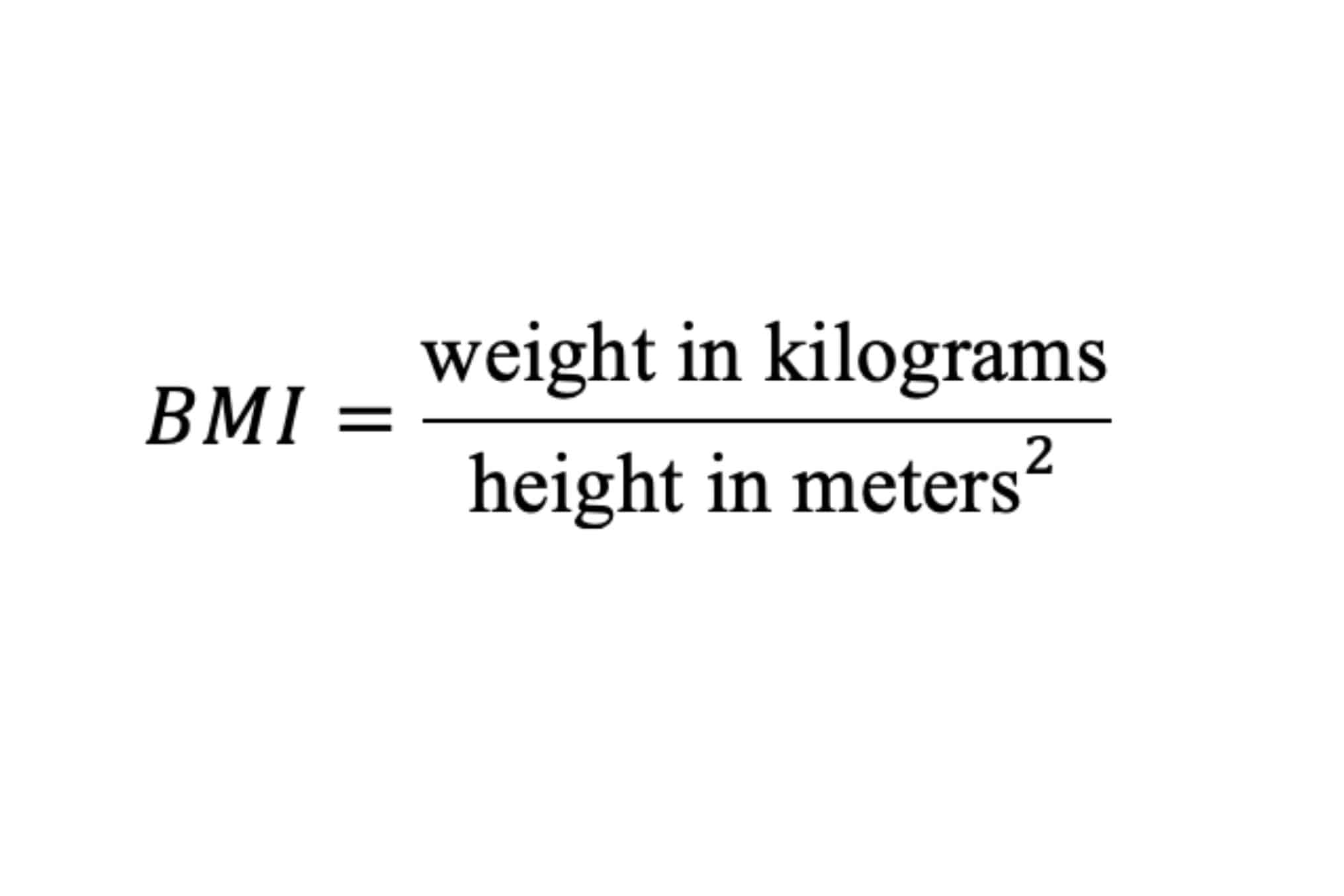
In the United States, BMI is often calculated using pounds and inches with a conversion factor, but the concept remains the same.
The resulting number is then placed into categories:
- Underweight: BMI less than 18.5
- “Normal” weight: BMI 18.5 to 24.9
- Overweight: BMI 25 to 29.9
- Obesity: BMI 30 or higher
These categories are used as general screening tools to identify potential health risks at a population level.
Why BMI Became So Widely Used
BMI gained popularity because it is simple, inexpensive, and easy to apply across large groups of people. It requires only two basic measurements and allows researchers and healthcare providers to track trends in weight-related health outcomes over time.
Public health organizations have used BMI to study associations between body size and conditions such as heart disease, type 2 diabetes, and certain cancers. Because of its convenience, it became a standard tool in clinical settings as well.
However, it’s important to understand that BMI was originally designed for population studies—not as a diagnostic tool for individual health.
What BMI Can Tell You
Despite its limitations, BMI can still provide some useful information when interpreted in context.
At a broad level, higher BMI ranges are associated with an increased risk of certain conditions, including cardiovascular disease, metabolic disorders, and joint issues. Lower BMI ranges may be associated with risks such as nutrient deficiencies or decreased bone density.
For example, in large-scale studies, populations with BMI values above 30 tend to have higher rates of type 2 diabetes. This doesn’t mean that every individual with a BMI above 30 will develop diabetes, but it highlights a statistical trend.
In this way, BMI functions best as a screening tool—something that can prompt further evaluation rather than serve as a final judgment.
The Limitations of BMI
While BMI is widely used, it has several well-documented limitations that make it an incomplete measure of individual health.
- It does not distinguish between fat mass and muscle mass; a muscular person may have a high BMI but low body fat
- It does not account for fat distribution, which plays a significant role in health risk
- It does not consider factors like age, sex, ethnicity, or genetics
- It cannot measure metabolic health, fitness level, or lifestyle behaviors
For instance, an athlete with high muscle mass might fall into the “overweight” or “obese” category based on BMI alone, despite having excellent cardiovascular health and metabolic markers.
BMI and Metabolic Health
One of the most important limitations of BMI is that it does not directly reflect metabolic health.
Metabolic health includes factors such as blood sugar levels, cholesterol, blood pressure, and insulin sensitivity. It is possible for someone with a higher BMI to have normal metabolic markers, and for someone within the “normal” BMI range to have underlying metabolic issues.
This is why many healthcare providers now look beyond BMI to assess health more comprehensively. Lab values, physical activity levels, diet quality, sleep, and stress all play a role.
BMI can be one piece of the puzzle—but it should not be the entire picture.
How BMI Intersects With Weight-Inclusive Care
In weight-inclusive care, BMI is often treated as a data point rather than a defining measure of health.
Instead of focusing solely on BMI categories, providers may prioritize behaviors and outcomes such as:
- Nutritional adequacy
- Physical activity
- Symptom management
- Mental well-being
- Quality of life
For example, a person with IBS might have a BMI in any category but still require specific dietary strategies, such as a low FODMAP approach, to manage symptoms. In this case, success is measured by reduced bloating, improved digestion, and better daily functioning—not by changes in BMI.
Save this article
This perspective helps reduce stigma while still allowing BMI to be used when appropriate.
When BMI Can Be Helpful in Clinical Contexts
Although BMI has limitations, it can still be useful in certain clinical situations—particularly when combined with other assessments.
Healthcare providers may use BMI as a starting point to:
- Identify potential risk factors that warrant further testing
- Guide conversations about overall health patterns
- Monitor population-level trends in clinical settings
In some cases, BMI may also be considered when determining eligibility for certain treatments or screenings. However, it is increasingly recognized that relying on BMI alone can lead to oversimplified or even misleading conclusions.
BMI and Special Populations
BMI does not apply equally across all populations, and its interpretation may need to be adjusted.
For example:
- Older adults may have different body composition and health risks at the same BMI
- Athletes often have higher BMI due to muscle mass
- Some ethnic groups may experience metabolic risks at lower BMI thresholds
- Children and adolescents use age- and sex-specific BMI percentiles rather than standard categories
These variations highlight the importance of individualized assessment rather than strict reliance on BMI cutoffs.
You might also want to read:
- Weight Management Series: How to Gain Weight on the Low FODMAP Diet
- Weight Management Series: How to Lose Weight on the Low FODMAP Diet
- 12 Common Foods To Skip If You Want A Longer Healthier Life
Common Misconceptions About BMI

BMI is often misunderstood, which can lead to confusion or unnecessary concern.
One common misconception is that BMI directly measures body fat. In reality, it is simply a ratio of weight to height and does not assess body composition.
Another misconception is that BMI determines whether someone is “healthy” or “unhealthy.” Health is influenced by a wide range of factors, many of which are not captured by this single number.
There is also a tendency to view BMI categories as rigid or definitive. In practice, they are general guidelines that should be interpreted with flexibility and context.
How to Use BMI in a Balanced Way
If you encounter your BMI in a medical setting or online calculator, it can be helpful to view it as one piece of information rather than a final verdict.
A balanced approach might include:
- Looking at additional health markers, such as blood pressure, cholesterol, and blood sugar
- Considering lifestyle factors like diet quality, movement, sleep, and stress
- Reflecting on how you feel physically and mentally
- Discussing results with a healthcare provider who takes a holistic view
For individuals managing specific health conditions—such as digestive disorders requiring structured dietary approaches like low FODMAP—focusing too heavily on BMI can distract from more meaningful goals, like symptom relief and nutritional adequacy.
The Future of BMI in Health Care
As understanding of health becomes more nuanced, the role of BMI is evolving. Many experts continue to use it for large-scale research and initial screening, while also advocating for more comprehensive and individualized assessments.
Emerging approaches emphasize a broader view of health—one that includes metabolic markers, behavior patterns, social determinants, and patient experience. In this context, BMI is no longer seen as the defining measure, but rather as one tool among many.
This shift reflects a growing recognition that health cannot be reduced to a single number. By understanding both the value and the limitations of BMI, individuals and providers can use it more thoughtfully—without letting it overshadow the bigger picture.
Disclosure: This article was developed with the assistance of AI and was subsequently reviewed, revised, and approved by our editorial team.
Like our content? Follow us on Newsbreak.
For decades, health advice has centered on one goal: lose weight. That idea is now being challenged.

A growing shift in healthcare is challenging the long-held belief that weight loss defines health, replacing it with a broader, evidence-driven focus on well-being.
A growing number of clinicians and researchers are shifting toward a more comprehensive view of health, one that looks beyond body size. Instead of focusing primarily on weight loss, this approach emphasizes sustainable habits, metabolic health, and overall well-being. Learn more.






