“Leaky gut”, or increased intestinal permeability, is a common problem for anyone suffering from digestive and autoimmune conditions. Not all doctors agree yet on whether this problem really exists or its relationship to other conditions.
Fortunately for us, the evidence continues to accumulate as researchers look for more answers.
To better understand what “leaky gut” is, try to visualize your digestive tract as a long tube that connects your mouth to your anus. This tube has a very thin lining, in fact, it’s only about 3 mm thick or about the width of two pennies.
This lining is essential for keeping food particles inside the intestine and also for making it possible to absorb nutrients from the food we eat.

Standard American Diets Don’t Help
There are very small spaces between the cells in the lining, called tight junctions, that can sometimes become compromised. Eating a Standard American Diet (SAD) that is full of processed, low fiber foods can have a negative effect on the integrity of the lining along with stress, medications, alcohol, and food allergies to name a few.
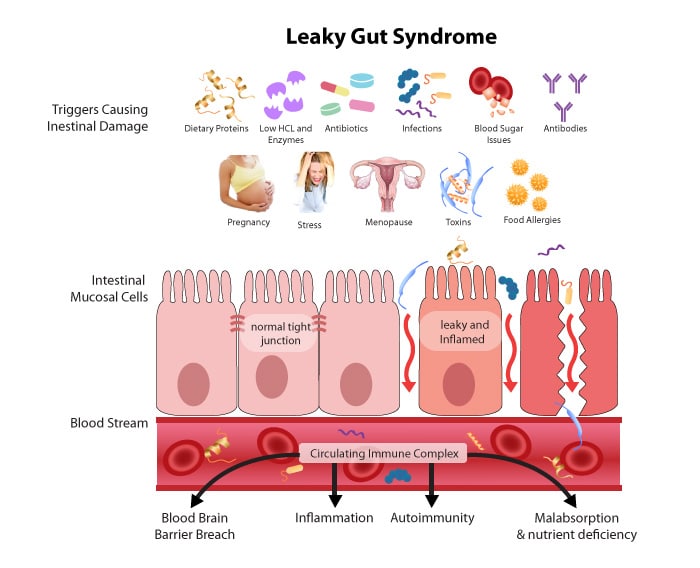
Once these spaces grow in size, it’s easy for bacteria or partially digested proteins and fats to sneak out of the intestine and into the circulation of the body. Once in the blood stream, the immune system reacts to these foreign materials.
The Gluten – Zonulin Connection
We can’t talk about leaky gut without addressing zonulin. Zonulin is a protein, that has been identified in recent years, which increases intestinal permeability by opening up the spaces between the cells in the intestine. So, what causes too much zonulin in our guts?
So far, researchers have identified that gliadin, a protein found in gluten, can increase zonulin levels along with harmful bacteria or yeast found in the intestine. This is an exciting area of research as more is learned about this response and potentially other pathways that might affect intestinal permeability.
Symptoms of Leaky Gut
The symptoms that may be associated with leaky gut are numerous and could be easily related to other conditions. Some of the most common include:
- Bloating
- Abdominal pain
- Diarrhea
- Fatigue
- Food intolerances
- Skin rashes
- Poor exercise tolerance
- Cognitive and memory deficits
Save this article
Conditions Associated with Leaky Gut
There are many conditions that may have an association with leaky gut. Some common ones include:
- Acne
- Celiac disease
- Eczema
- Inflammatory bowel disease (Crohn’s disease, ulcerative colitis)
- Irritable bowel syndrome
- Multiple food and chemical sensitivities
How to Test For It
There are several ways to test for leaky gut. One of the most common methods is the lactulose/mannitol urine test. This is a simple, non-invasive test that measures the amount of specific sugars in your urine.
Using this information, a ratio is calculated that can give you an idea of whether leaky gut is present or not.
Many practitioners choose not to use a clinical test, however. As you can see from the list of symptoms and related conditions, healing the gut lining becomes important for most digestive problems.
How to Heal Your Intestines
Working with a dietitian can help as you try to discover foods that might be triggering symptoms and thus may be causing leaky gut. The low FODMAP diet is a great tool that can be used to make this process easier.
The body has an amazing ability to heal itself. One of the first steps in overcoming leaky gut is to figure out what could be causing the condition. You may choose to work on managing your stress or trying a gluten-free diet to improve your gut health.
It’s pretty remarkable that once triggers are taken away, the cells found in the wall of the intestine can actually regenerate themselves.
You May Want To Read: What Is Leaky Gut Syndrome?
And if you want personal help with your digestive issues, consider working remotely with a FODMAP savvy dietitian like Joe Leech and his team. They have courses and 1 on 1 options for you.
References
- Fasano, Alessio. “Intestinal Permeability and Its Regulation by Zonulin: Diagnostic and Therapeutic Implications.” Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association 10.10 (2012): 1096–1100. PMC. Web. 24 May 2017.
- Fasano, Alessio. “Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer.” Physiological reviews 91.1 (2011): 151-175.
- Liska, DeAnn., and Jeffrey Bland. Clinical Nutrition: A Functional Approach. 2nd ed. Gig Harbor, Wash.: Institute for Functional Medicine, 2004.
- Mishra, Asha, and Govind K Makharia. “Techniques of Functional and Motility Test: How to Perform and Interpret Intestinal Permeability.” Journal of Neurogastroenterology and Motility 18.4 (2012): 443–447. PMC. Web. 24 May 2017.








