Meet Jody Garlick, RDN, LDN
Jody Garlick is an RDN, LDN practicing in the Pittsburgh, PA area. She is part of the FODMAP Everyday Team as a Contributor and you can read more about her on that page.
We first came across Jody’s work through her books on Amazon that cover the low-FODMAP diet for vegetarians, holiday dishes, smoothies and her work in the FODMAP diet world.
We chatted with Jody about her work as a dietitian and particularly about her work with the low-FODMAP diet and her patients to bring you this Q&A.
Dédé: Jody, you have been a practicing dietitian for years. Tell us how you first came across the low-FODMAP diet and was it something that you applied immediately in your practice?
Jody: I first learned about the diet several years ago when I was studying integrative and functional nutrition. I didn’t use it right away with clients because it seemed very restrictive and I wasn’t sure it was effective. I tend to wait a while before trying anything new with clients. As more research became available and I saw more dietitians were using the low-FODMAP diet, I felt comfortable using it with clients. Looking back, I wish I would have introduced it sooner because it’s been an invaluable tool for my clients to manage IBS.
This was exactly my impetus for creating FODMAP Everyday. Once I experienced relief through the diet I wanted to spread the word far and wide! What was your initial impression with patients? How did they receive the low-FODMAP diet information and what techniques did you develop to help them understand and follow the diet?
The low-FODMAP diet is more common now and my clients often have some idea of what types of restrictions are involved. When I first started using it, that wasn’t the case. Many of my clients were shocked by how many foods were high in FODMAPs, but once they gave it a chance, the symptom relief for most was worth the sacrifice.
With any type of elimination diet, I try to help my clients focus on the positive (what they can eat) and encourage them to try new things. My philosophy is that any diet change should done slowly to let the body adjust, so I encourage people to use baby-steps when starting the low-FODMAP diet.
When a doctor tells someone they should try the low-FODMAP diet and to go find a RDN, what should the patient look for? You, for instance, consider yourself as outside the box and take a fairly integrative approach. Can you talk a little bit about how someone can find the right RDN for them and also a bit about your methodology?
In looking for a RDN, I would suggest finding someone who not only teaches the low-FODMAP diet, but also specializes in digestive health. There are often multiple issues going on with clients and it’s rarely a simple case of IBS and a low-FODMAP diet to manage it. Integrative dietitians have additional training and use a combination of conventional and complementary therapies to help clients achieve goals.
This type of approach is more patient-centered and healing oriented. An example of how I might use this methodology for a client with IBS would be creating a nutrition plan that includes: a therapeutic low-FODMAP diet, dietary supplements, and yoga along with continuing any medications prescribed by a physician and including the physician in any follow-up care.
Most importantly, though, is to allow my clients to be in control of what types of therapies are included and what goals are created.
I love this answer as you have rolled so many important points into one: not every RDN is FODMAP savvy but more and more are and with telehealth options, you do not have to necessarily limit yourself to your own locale.
The diet can seem daunting at first. What is the most helpful thing that you share with patients who you think should try the low-FODMAP diet?
It’s so hard for people to remember which foods are low-FODMAP and especially the serving sizes. There are a couple of great apps that can be used to reference this information quickly and easily. My favorite is the low-FODMAP diet app created by Monash University. It’s like having a cheat sheet with you all the time and allows for easy reference when dining out or grocery shopping.
I am never without my Monash University app; I couldn’t agree more and I reference it daily. Knowing that you have information literally at hand that is completely trustworthy goes a long way to not only to helping logistically but also for peace of mind.
Where are the sticking points for patients once they start? Do you see any consistency as to where there are points of difficulty?
There is definitely a learning curve for many at the start. It’s so hard giving up the foods that we love. Clients who are able to find replacements for those favorite foods seem to have an easier time moving forward. I also notice that certain challenge weeks are more difficult.
The fructans and lactose groups are by far the toughest for most. Working one-on-one with a registered dietitian who can also help motivate through the tough periods, can help make the process easier.
Save this article
Let’s talk vegetarians – after all you wrote a book geared towards vegetarians and the low-FODMAP diet. What vegetarians who are embarking on the low-FODMAP diet?
A concern for vegetarians is getting adequate protein and the low-FODMAP diet can make this more challenging. I encourage vegetarians to focus on using canned lentils rather than dried because of the lower FODMAP content for a great source of protein and iron.
Another option is to add a chopped, hard-cooked egg to a meal for additional protein. Another great tip for vegetarians is to make the most of firm tofu. This is something that can be kept on hand and makes a quick meal.
I love to cut it into strips and marinate it before cooking it on the grill with some vegetables.
Any particular tips for vegans?
Vegans tend to have trouble getting enough calcium. Rather than use almond milk purchased from the store, I suggest clients try making it to use with a smoothie. A serving of almonds (10) can be soaked overnight and then drained in the morning.
The nuts can be added to a high-speed blender with a cup of water and blended until smooth. The calcium found naturally in almonds is much easier for the body to absorb than what is added to fortified almond milk.
You just made the concept of homemade almond milk super easy; I hope folks try that!
Holidays are synonymous with food and holiday parties can be hard to navigate when you are being mindful of restrictions. Tell us about your book focusing on holidays and some of your best tips and tricks.
It seems that any sort of social gathering involving food can be difficult for anyone following a special diet. This is especially hard when someone is just starting a low-FODMAP diet and still a bit anxious about how to navigate it.
My favorite way to overcome this situation is to get in touch with the host and ask what will be served and offer to bring a special dish or appetizer that will complement the meal. Although this can be tough to do the first time, I can’t imagine going to any function now without asking first!
One of my favorite recipes from my book that I like to take to holiday gatherings is the No Crust Pumpkin Pie. It’s so easy to make and is just as delicious without the crust.
Summer is around the corner and all that fresh fruit is going to hit the farmer’s markets. You are a smoothie aficionado and we would love to hear about your low-FODMAP approach. And this is a perfect time to hear how you help your patients with serving size guidelines.
My Vitamix is probably my favorite appliance and I do love developing new smoothie recipes. This can be a tricky area for people following a low-FODMAP plan, but that doesn’t mean it can’t be done.
I use a step-by-step approach to teaching clients how to be successful in sticking to the FODMAP portion sizes when building smoothies. They start with a non-dairy or lactose-free base, add a low-FODMAP serving of fruit, a protein choice, a nutrient booster such as ginger or spinach, and an optional sweetener.
I provide them with a guide to use until they get the hang of it and then the possibilities are endless!
Jody, thank you so much for this chat. We know that you are invested in helping IBS sufferers thrive on the low-FODMAP diet; we need more RDNs like you!
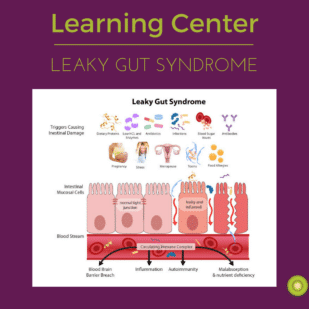
You might like Jody’s introductory article on leaky gut.