Have you ever wondered about these two conditions? Although irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD) sound similar, they actually couldn’t be more different.
If you or someone you care about is suffering from IBS or IBD, this article will teach you about each of these conditions, the diagnosis process, and approaches to managing them.
Description Of IBS and IBD
Irritable bowel syndrome, or IBS, used to be called a functional digestive disorder, or FGID, but is now more often referred to as a disorder of gut-brain interaction, or DGBI. Physically, the digestive tract looks normal, but there’s a problem in the way it works. IBS is characterized by altered bowel movements and abdominal pain. Other common symptoms include gas and bloating.
Surprisingly, IBS affects about 10 to 15% of the world population and is more prevalent in women than men. For more info on IBS you can read that here.

On the other hand, inflammatory bowel disease, or IBD, is an autoimmune condition characterized by chronic intestinal inflammation. There are physical changes that can be seen in the digestive tract due to the ongoing inflammation.
The most common forms of IBD are Crohn’s disease and ulcerative colitis. IBD is a much more serious condition that has some long-term issues including:
- Micronutrient deficiencies
- Weight loss
- Malnutrition
Impact On Life
What these two conditions do have in common is the effect the symptoms can have on a person’s life. They both can cause chronic, often long-term problems such as:
- Absenteeism from work
- Poor quality of life
- Often high health costs
Diagnosis Of IBS and IBD
Unfortunately, the process for diagnosis of irritable bowel syndrome can be quite frustrating. Since there isn’t one specific test to diagnose it, doctors must first rule out more serious conditions such as celiac disease, IBD, small intestinal bacterial overgrowth (SIBO), diverticulitis, endometriosis, and other medical conditions.
It is vitally important to get an accurate diagnosis before developing a treatment plan.
If those conditions (and others) are ruled out, doctors can diagnose functional gastrointestinal disorders like IBS based on symptoms and stool patterns.
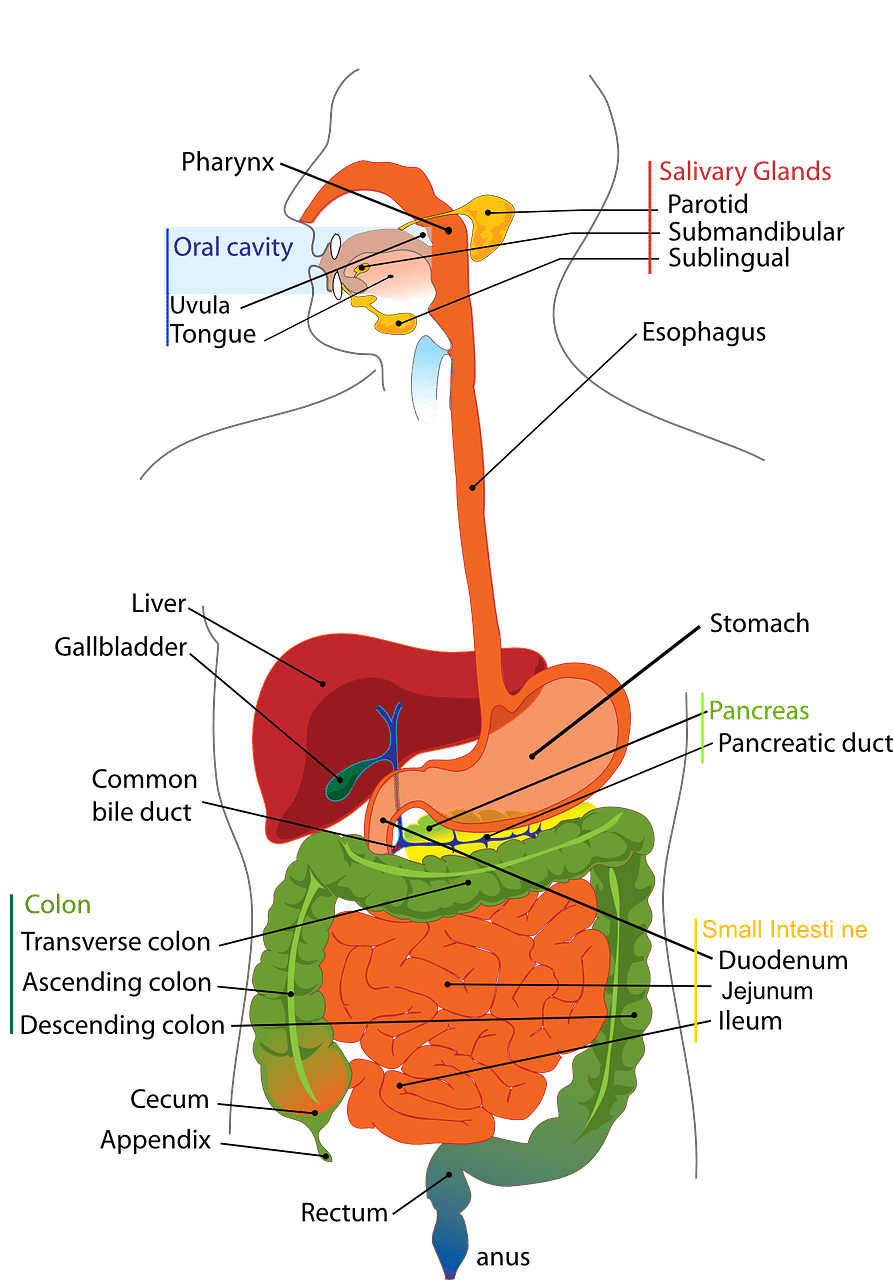
Inflammatory bowel disease can be equally difficult to diagnose, but there are specific diagnostic tests that are performed to confirm it. Blood and stool tests are used initially to look for markers of inflammation. To get a better look at the digestive tract, doctors use endoscopy and colonoscopy.
Sometimes the inflammation doesn’t show up in testing initially and may take repeated attempts before getting a diagnosis.
Save this article
You may want to read: IBS: Step-by-Step Guide from Diagnosis to Symptom Free Living
Treatment Of IBS and IBD
At this time, IBS and IBD cannot be “cured,” but there are different methods for controlling symptoms and managing the conditions. Approaches may include medications, special diets, supplements, and mind-body techniques.
- DIET: One of the most promising methods for controlling symptoms of IBS is the low FODMAP diet. In fact, this diet has been shown to improve symptoms for 3 out of 4 people who follow it. While it’s not a cure, it gives people a way to control symptoms and helps overall management of this disorder. This means a better quality of life, missing less work, and possibly spending less on health care costs. You may want to read: Can The Low FODMAP Diet Help My IBD?
- PROBIOTICS: Some practitioners are hopeful that someday there may be specific probiotic supplements that will be used for targeted treatment in IBS and IBD. This is an area of research that is currently evolving and we continue to learn more each day.
- STRESS REDUCTION: Stress management techniques like meditation are also quite helpful in managing IBS symptoms. A study published in The American Journal of Gastroenterology showed a reduction in IBS symptom severity following 8 weeks of using mindfulness meditation. With this type of meditation, attention is focused on present experiences and being aware of how the body feels and emotions that are present.

- MEDICATIONS: IBD is often controlled with the use of medications, but the role of diet in the management of this condition is becoming more popular. Since many people with IBD also suffer from IBS-like symptoms such as gas, bloating, and abdominal pain, along with fructose and lactose malabsorption, the low FODMAP diet is a tool to consider in managing this condition. It’s important that this type of restrictive dietary intervention be implemented with the help of a dietitian since undernutrition is commonly a problem for those with IBD.
Putting It All Together
Even though IBS and IBD are quite different conditions, they do share some similarities. Either one can cause long-term symptoms and decrease quality of life for people, but fortunately, there are a variety of ways to manage either condition.
Diet is becoming a more popular approach as the evidence to support it continues to evolve. It’s nice to see more people finding relief from their symptoms by using “food as medicine.”
Other articles you may want to read:
- What If I Have Both IBS and IBD?
- Can A Low FODMAP Diet Help My IBD?
- Differentiating IBS from Colon Cancer: Symptoms and Diagnosis
- Pancreatic Cancer, Pancreatitis and IBS Connection: Don’t Let Your Symptoms Go Unchecked
References
Campbell, Kristina, et al. Diet and Probiotics Emerge as Promising Treatments . Gut Microbiota for Health, 3 Feb. 2016, www.gutmicrobiotaforhealth.com/en/in-new-understandings-of-ibs-diet-and-probiotics-emerging-as-promising-treatments/.
Campbell, Kristina, et al. Exploring the Clinical Usefulness of the Low-FODMAP Diet for Crohn’s Disease. Gut Microbiota for Health, 12 Sept. 2016, www.gutmicrobiotaforhealth.com/en/exploring-clinical-usefulness-low-fodmap-diet-crohns-disease/.
Diet and Inflammatory Bowel Disease. Gastroenterology Hepatology, www.gastroenterologyandhepatology.net/archives/august-2015/diet-and-inflammatory-bowel-disease/.
Gaylord SA, Palsson OS, Garland EL, et al. Mindfulness training reduces the severity of irritable bowel syndrome in women: results of a randomized controlled trial. The American Journal of Gastroenterology. 2011;106(9):1678-1688.
Gibson, Peter R. Use of the Low‐FODMAP Diet in Inflammatory Bowel Disease. Journal of Gastroenterology and Hepatology, 28 Feb. 2017, onlinelibrary.wiley.com/doi/10.1111/jgh.13695/full.
Matarese, Laura E., et al. The Health Professional’s Guide to Gastrointestinal Nutrition. Academy of Nutrition and Dietetics, 2015. Print.