Despite overlapping symptoms that blur the lines for millions of patients, irritable bowel syndrome and diverticulitis remain fundamentally different conditions with distinct risks, causes, and consequences.
Irritable bowel syndrome (IBS) and diverticulitis overlap in ways that make them easy to confuse. Both can involve abdominal pain, disrupted bowel habits, and unpredictable flare-ups that interfere with daily life, with a level of unpredictability that can be frustrating and even frightening.
While there are these overlaps of symptoms, they are not the same condition, they do not share the same cause, and having one does not automatically mean you will develop the other.
This article walks you through what we actually know, what the research says, and how to interpret the overlap in a way that is grounded in science.
- Understanding IBS: A Gut-Brain Disorder
- Understanding Diverticular Disease
- How Common Is Diverticulitis?
- Do People With IBS Get Diverticulitis More Often?
- Why Do These Conditions Get Confused?
- When IBS Is Not IBS
- The Concept of Post-Diverticulitis IBS
- Shared Risk Factors and Misconceptions
- The Role of Inflammation
- IBS vs. Diverticulitis Treatment
- Age as a Key Factor
- What About the Microbiome?
- Practical Takeaways
- A More Reassuring Perspective
Understanding IBS: A Gut-Brain Disorder
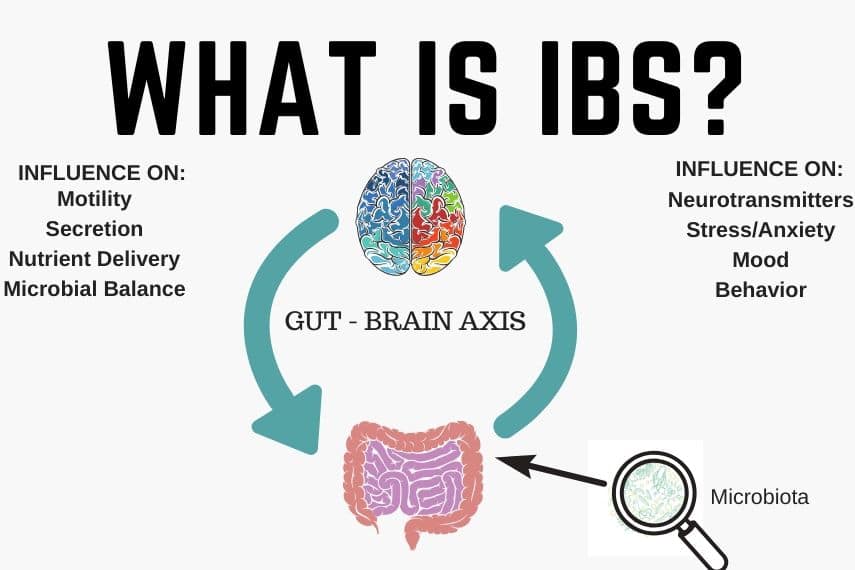
Irritable Bowel Syndrome is classified as a functional gastrointestinal disorder, and used to be referred to as a “FGID”. Today, IBS is referred to as a disorder of gut-brain interaction or “DGBI.” That language matters.
With IBS, there is no structural damage visible on imaging or colonoscopy. Instead, the issue lies in how the gut and nervous system communicate.
People with IBS may experience:
- Abdominal pain that improves or worsens with bowel movements
- Bloating and visible distension
- Diarrhea (IBS-D), constipation (IBS-C), or a mix of both (IBS-M)
- Heightened sensitivity to normal digestive processes (Visceral Hypersensitivity)
The condition is chronic, meaning it tends to come and go over time rather than resolve completely. There is no cure for IBS.
IBS affects approximately 10 to 15 percent of adults in the United States (4 to 15 percent globally), making it one of the most common gastrointestinal conditions seen by primary care providers and gastroenterologists.
Understanding Diverticular Disease
To understand diverticulitis, we need to start with its precursor.
Diverticulosis refers to the presence of small pouches that form in the wall of the colon. These pouches are called diverticula.
They are extremely common, especially with aging. Many people have diverticulosis and never know it because it often causes no symptoms. In this sense, it is similar to what happens with the gallbladder. You can have stones in your gallbladder, but not have symptoms, and therefore it is not a problem.
Estimates suggest:
- About one third of people over age 60 have diverticulosis
- Up to two thirds of people over age 80 have it
Most people with diverticulosis will never develop complications. However, a subset will go on to develop inflammation or infection of these pouches.
That condition is called Diverticulitis.
Diverticulitis is very different from IBS. It is an acute inflammatory condition that can range from mild to severe.
Symptoms typically include:
- Sharp abdominal pain, often on the lower left side
- Fever
- Nausea and vomiting
- Changes in bowel habits
- Elevated white blood cell count
Unlike IBS, diverticulitis can require antibiotics, imaging, hospitalization, and in severe cases, surgery.
How Common Is Diverticulitis?

Although diverticulosis is very common, diverticulitis is less so.
- Older estimates suggested that 10 to 25 percent of people with diverticulosis would develop diverticulitis. More recent research has revised that number downward.
- Current data suggest that approximately 4 to 15 percent of people with diverticulosis will develop diverticulitis over their lifetime.
That distinction is important. Having diverticula does not mean you will develop inflammation or infection.
Do People With IBS Get Diverticulitis More Often?
The short answer is no. There is no strong evidence that having IBS significantly increases your risk of developing diverticulitis.
Several studies have examined this relationship and found that while the two conditions can coexist, IBS is not considered a risk factor for diverticulitis in the way that aging or certain lifestyle factors are.
This means there is no reliable statistic such as a specific percentage of IBS patients who will develop diverticulitis. The overlap exists, but it is not driven by a direct causal relationship.
Why Do These Conditions Get Confused?
If IBS and diverticulitis are so different, why are they so often linked in conversation?
The answer comes down to symptom overlap.
Both conditions can cause:
- Abdominal pain
- Bloating
- Changes in bowel habits
- Periods of flare and remission
From a patient perspective, it can feel like the same problem behaving differently.
From a clinical perspective, the underlying mechanisms are entirely different.
IBS involves altered motility, visceral hypersensitivity, and gut-brain signaling.
Diverticulitis involves localized inflammation and sometimes infection of a structural abnormality in the colon.
The confusion is understandable, but it can also be risky if it leads to misinterpretation of symptoms. This is one of the many reasons why no one should self-diagnose.
When IBS Is Not IBS

One of the most important distinctions for anyone living with IBS is recognizing when symptoms fall outside the typical pattern.
IBS does not cause fever.
IBS does not cause elevated inflammatory markers.
IBS does not cause complications like abscesses or perforation.
If someone with IBS suddenly experiences:
- Persistent, localized abdominal pain
- Fever or chills
- Nausea and vomiting
- Pain that does not improve after a bowel movement
That should not be dismissed as a typical IBS flare. It warrants medical evaluation to rule out diverticulitis or another condition.
The Concept of Post-Diverticulitis IBS
There is one area where the relationship between these conditions becomes more nuanced.
Some people who have had an episode of diverticulitis go on to develop chronic gastrointestinal symptoms that resemble IBS.
This is sometimes referred to as post-diverticulitis IBS or post-inflammatory IBS.
After the acute inflammation resolves, patients may continue to experience:
- Ongoing abdominal discomfort
- Altered bowel habits
- Heightened sensitivity in the gut
This is similar to what is seen after infectious gastroenteritis, where a subset of individuals develops post-infectious IBS.
In this case, the sequence is reversed. The structural inflammatory event comes first, followed by functional symptoms.
Shared Risk Factors and Misconceptions
Although IBS does not cause diverticulitis, the two conditions can share certain overlapping factors that contribute to confusion.
Diet
Diet is one of the most commonly discussed areas.
Historically, people with diverticulosis were advised to avoid nuts, seeds, and popcorn based on the belief that these foods could lodge in diverticula and cause inflammation. That recommendation has largely been debunked.
At the same time, diet plays a major role in IBS symptom management, particularly through approaches such as the low FODMAP diet.
This creates a situation where individuals may assume that dietary triggers for IBS are also triggers for diverticulitis, which is not necessarily the case.
Bowel Habits
Another shared factor is bowel habit variability.
Constipation can be present in both IBS and diverticular disease. Chronic constipation is considered a potential risk factor for diverticular complications because it increases pressure within the colon.
However, IBS-related constipation does not automatically translate into diverticulitis risk.
The Role of Inflammation

One of the clearest differences between IBS and diverticulitis is the presence or absence of inflammation.
IBS is not an inflammatory disease in the traditional sense. While there may be subtle immune activation in some cases, it does not produce the kind of measurable inflammation seen in diverticulitis.
Diverticulitis, on the other hand, is defined by inflammation.
This distinction is why blood tests, imaging, and physical examination findings are so important when evaluating abdominal pain.
IBS vs. Diverticulitis Treatment
It also explains why treatments differ so dramatically.
- IBS management focuses on diet, stress modulation, and sometimes medications that affect gut motility or sensitivity.
- Diverticulitis treatment may involve antibiotics, bowel rest, and in severe cases, surgical intervention.
Age as a Key Factor
Age plays a major role in diverticular disease and much less so in IBS.
IBS often begins in younger adulthood and can persist for decades, and/or can take many years to diagnose properly.
Diverticulosis and diverticulitis become more common with age, particularly after age 50.
This means that some individuals may have IBS for many years and then later develop diverticulosis simply due to aging.
If diverticulitis occurs, it may be tempting to assume that IBS “turned into” diverticulitis, but that is not how the process works.
These are separate conditions that can appear in the same person at different points in life.
What About the Microbiome?

The gut microbiome is frequently discussed in both IBS and diverticular disease, and for good reason.
Alterations in gut bacteria have been implicated in IBS symptoms, particularly in relation to gas production, fermentation, and sensitivity.
There is also emerging research suggesting that changes in the microbiome may play a role in the development of diverticulitis, although this area is still evolving.
This shared area of research contributes to the perception that the conditions are closely linked.
However, similarity in research focus does not mean similarity in disease mechanism.
IBS remains a functional disorder of gut-brain interaction, while diverticulitis remains an inflammatory complication of structural changes in the colon. They can coexist, but one does not drive the other in a predictable or common way.
Practical Takeaways
For someone living with IBS, the most important points are straightforward.
- Having IBS does not mean you are likely to develop diverticulitis.
- There is no clear percentage or statistic linking the two conditions in a meaningful way.
- Symptom overlap can create confusion, but the underlying causes are different.
The most important practical skill is learning to recognize when symptoms fall outside your typical IBS pattern.
That awareness can help ensure that conditions like diverticulitis are identified and treated appropriately rather than being dismissed as another flare.
A More Reassuring Perspective
It is easy to fall into a mindset where every new or different symptom feels like a progression or complication of an existing condition.
In the case of IBS and diverticulitis, the data do not support that kind of progression.
Remember that IBS remains a functional disorder of gut-brain interaction, while diverticulitis remains an inflammatory complication of structural changes in the colon. They can coexist, but one does not drive the other in a predictable or common way.
Understanding that distinction can reduce unnecessary anxiety and help guide more appropriate responses to symptoms when they arise.
Sources
American Gastroenterological Association
AGA Clinical Practice Update on Medical Management of Colonic Diverticulitis
https://gastro.org/clinical-guidance/aga-clinical-practice-update-on-medical-management-of-colonic-diverticulitis/
Peery AF, et al. Burden of Gastrointestinal Disease in the United States.
Gastroenterology. 2015.
https://pubmed.ncbi.nlm.nih.gov/25618004/
Strate LL, Morris AM. Epidemiology, Pathophysiology, and Treatment of Diverticulitis.
Gastroenterology. 2019.
https://pubmed.ncbi.nlm.nih.gov/30660706/
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
Irritable Bowel Syndrome
https://www.niddk.nih.gov/health-information/digestive-diseases/irritable-bowel-syndrome
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
Diverticular Disease
https://www.niddk.nih.gov/health-information/digestive-diseases/diverticular-disease
Ford AC, Lacy BE, Talley NJ. Irritable Bowel Syndrome.
The Lancet. 2017.
https://pubmed.ncbi.nlm.nih.gov/28131536/
Spiller R, Garsed K. Postinfectious Irritable Bowel Syndrome.
Gastroenterology. 2009.
https://pubmed.ncbi.nlm.nih.gov/19549532/
Simrén M, et al. Intestinal Microbiota in Functional Bowel Disorders.
Gut. 2013.
https://pubmed.ncbi.nlm.nih.gov/23665968/






